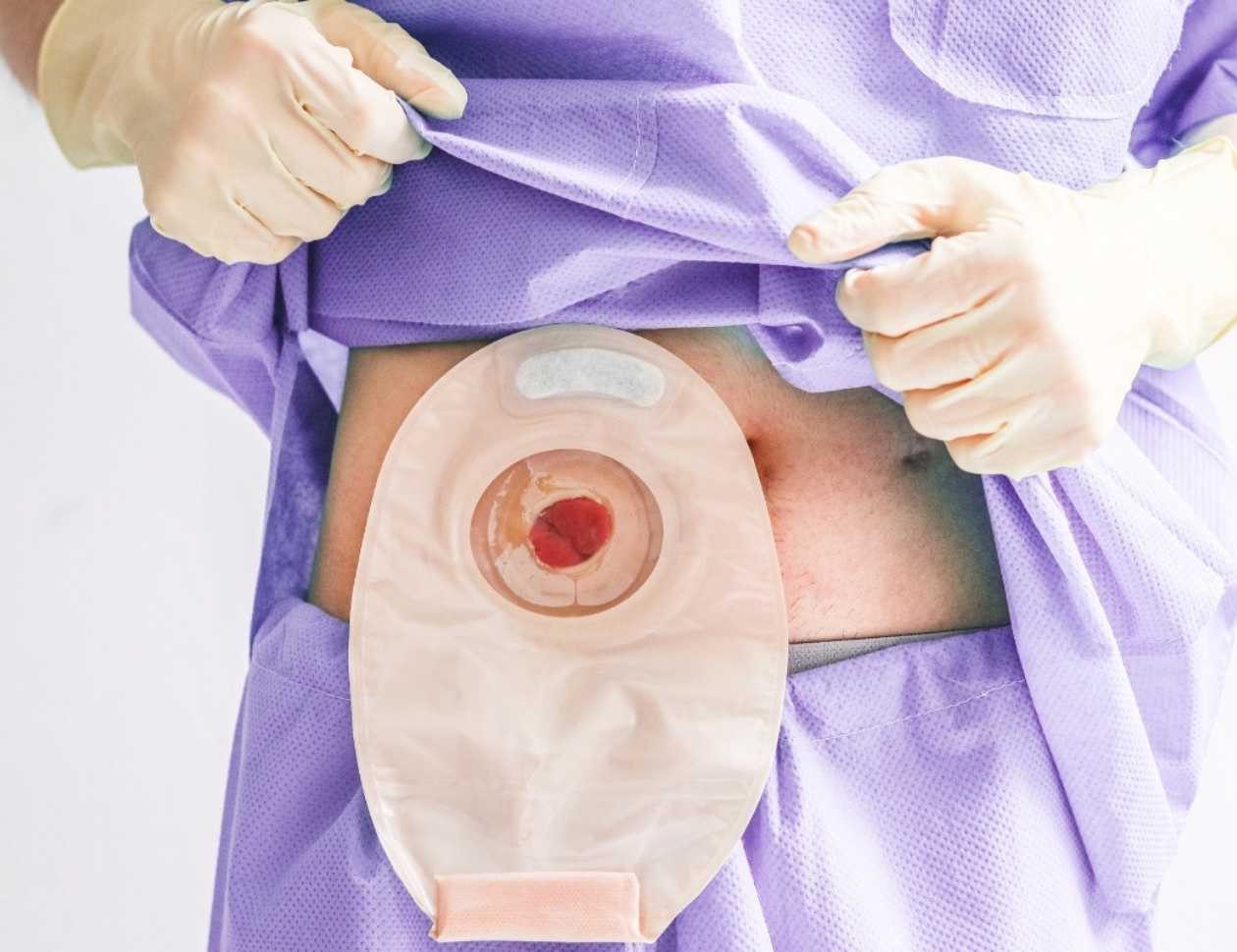
What Is a Stoma Bag?
During rectal cancer surgery, surgeons remove the cancer-affected portion of the rectum. In some situations, the bowel needs a temporary or permanent alternate exit pathway for stool.
This opening on the abdomen is called a stoma, and the pouch worn over it is known as a stoma bag (also called an ostomy bag).
There are two main types :
- • Colostomy – created from the large intestine (colon)
- • Ileostomy – created from the small intestine (ileum)
Both can be temporary or permanent, depending on the surgical and clinical situation.
Does Every Rectal Cancer Patient Need a Stoma?
No.
The need for a stoma depends on several important medical factors.
- 1. Location of the Tumour
This is the most critical factor.
Tumours located very low in the rectum — close to the anal sphincter muscles — are technically more challenging. If cancer involves the sphincter, preserving normal bowel control may not be possible, and a permanent stoma may be required.
However, many tumours are located higher up, allowing surgeons to safely reconnect the bowel.
- 2. Stage and Size of the Cancer
• Early-stage cancers are far more likely to be treated without a permanent stoma.
• Advanced cancers that invade nearby structures may require more extensive surgery.
- 3. Response to Pre-Surgery Treatment
Many patients receive chemotherapy and/or radiation before surgery (neoadjuvant therapy).
This treatment can shrink the tumour significantly. In some cases, it makes stoma-free surgery possible — even when it initially seemed unlikely.
In select patients where the tumour disappears completely, surgery may even be avoided through a carefully monitored "Watch and Wait" approach.
- 4. Patient’s Overall Health
Age, medical conditions, and baseline bowel function all influence surgical planning.
- 5. Surgeon’s Expertise and Technique
This is extremely important.
Specialised rectal cancer surgeons using advanced laparoscopic and robotic techniques have significantly higher rates of sphincter preservation and lower permanent stoma rates.
If you're consulting the Best Rectal Cancer Treatment Doctor in Max Hospital Dwarka, you can expect a treatment plan designed to maximise cancer control while preserving quality of life whenever possible.
What Do the Statistics Show?
Modern data is reassuring:
- 80–90% of colorectal cancer patients do NOT require a permanent stoma.
- A large U.S. study (2015–2018) showed only about 21% of rectal cancer surgery patients required a permanent stoma.
- In specialised high-volume centres using advanced protocols, permanent stoma rates have dropped to single-digit percentages.
Two decades ago, nearly half of rectal cancer patients required colostomy. Today, that number has dramatically reduced due to:
- • Better MRI imaging
- • Pre-operative chemoradiation
- • Precision surgery
- • Robotic-assisted techniques
Temporary vs Permanent Stoma: What’s the Difference?
Temporary Stoma
- • Created to protect a bowel join (anastomosis) while it heals
- • Usually reversed after 6 weeks to 6 months
- • Most common type in rectal cancer surgery
Permanent Stoma
- • Required when bowel reconnection isn’t possible
- • Usually when tumour involves the sphincter muscles
- • Patients can still enjoy excellent quality of life
Most stomas created during rectal cancer surgery are temporary, not permanent.
The Game-Changer: Sphincter-Sparing Surgerye
One of the most important advancements in rectal cancer care is Low Anterior Resection (LAR) — a sphincter-preserving procedure.
This technique allows surgeons to:
- • Remove tumours in the lower rectum.
- • Preserve the anal sphincter.
- • Avoid permanent colostomy in most cases.
With robotic-assisted and minimally invasive surgery, access to the deep pelvis has become far more precise.
If you are evaluating options with the Best Rectal Cancer Treatment Doctor in Max Hospital Dwarka, sphincter preservation is always carefully considered whenever oncologically safe.
Can Surgery — and a Stoma — Be Avoided?
In select patients who achieve complete tumour response after chemoradiation, a non-operative “Watch and Wait” strategy may be considered.
This approach:
- • Avoids immediate surgery
- • Requires strict follow-up and surveillance
- • Is suitable only for carefully selected cases
This represents a major shift in modern rectal cancer management.
Life With a Stoma: What Patients Should Know
If a stoma is needed — temporary or permanent — it does not mean life is limited.
With modern pouching systems and trained stoma care nurses, patients:
- • Return to work
- • Travel and exercise
- • Swim and wear normal clothing
- • Maintain full social and professional lives
Nearly one million people in the U.S. live with an ostomy. Quality of life remains high with proper support and education.
The Bottom Line
Rectal cancer surgery has transformed dramatically over the past two decades. For most patients, a permanent stoma is not inevitable.
The key factors are :
- • Early diagnosis
- • Proper staging
- • Multidisciplinary planning
- • Expertise of the surgical team
Every case is unique — and treatment should be personalised.
If you or a loved one has been diagnosed with rectal cancer, early consultation gives you more options and better outcomes
Conclusion
Rectal cancer treatment today is highly advanced, personalised, and focused not just on curing cancer, but also on preserving quality of life. In the majority of cases, a permanent stoma can be avoided with proper staging, modern techniques, and expert surgical care.
If you are seeking expert guidance, Dr. Sanjeev Kumar brings over 15 years of surgical oncology experience. He is among the few specialists in North India with dedicated expertise in gastrointestinal oncology, colorectal and pelvic cancers, robotic surgery, advanced laparoscopic surgery, and HIPEC / PIPAC procedures.
With the right specialist and a personalised treatment plan, better outcomes — and stoma-free surgery whenever safely possible — are achievable.